Understanding the shift—and what it means for your long-term health
You’re eating well. You’re exercising. You’re doing “all the right things.”
And then suddenly… your blood pressure starts creeping up.
If you’re in your 40s or 50s, this is incredibly common—and importantly, it’s not random.
Midlife, particularly the perimenopausal and menopausal transition, is a turning point for cardiovascular and metabolic health. Blood pressure often becomes one of the earliest signals that something deeper is shifting.
Let’s break down why this happens—and why it matters.
What is “normal” blood pressure?
Blood pressure is the force of blood pushing against your artery walls.
It’s measured with two numbers:
- Systolic (top number): pressure when the heart beats
- Diastolic (bottom number): pressure between beats
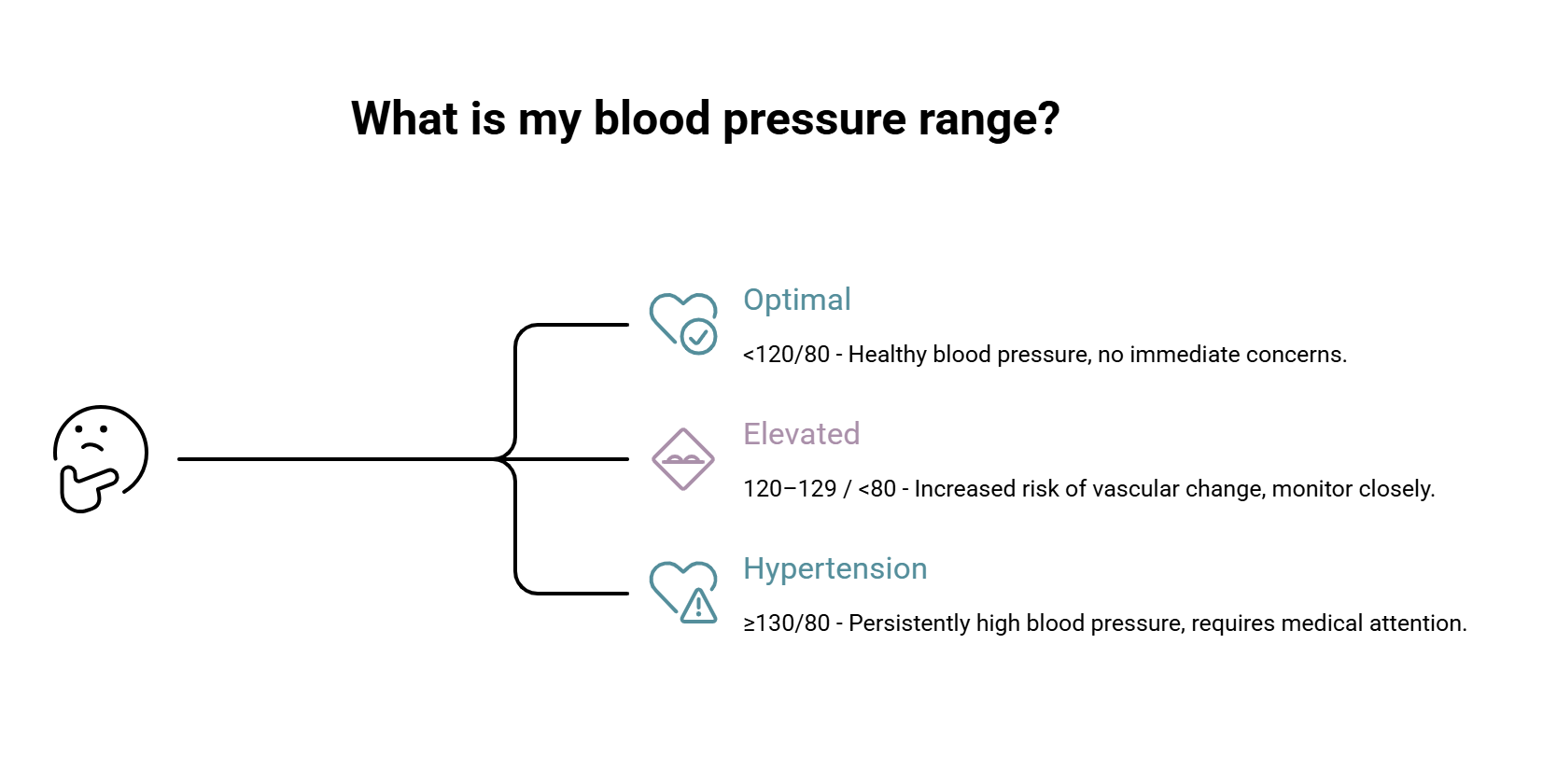
Healthy ranges:
- Optimal: <120/80
- Elevated: 120–129 / <80
- Hypertension: ≥130/80 (persistently)
Even being in the “elevated” range is not benign—it’s often the beginning of vascular change.
Why blood pressure rises in midlife
-
Loss of estrogen’s protective effects
Estrogen plays a major role in cardiovascular health. It helps:
- Keep blood vessels relaxed (vasodilation)
- Support healthy cholesterol balance
- Reduce inflammation in the vascular system
As estrogen declines:
- Blood vessels become stiffer and narrower
- Resistance increases → blood pressure rises
This is one of the key reasons why:
- Women often have lower BP than men earlier in life
- But surpass men in hypertension rates after menopause
-
Arterial aging + vascular stiffness
With age, arteries naturally lose elasticity.
This means:
- The heart must pump harder
- Pressure inside vessels increases
This process accelerates in midlife, especially when combined with hormonal shifts
-
Metabolic changes (this is a big one)
Midlife is also when we see:
- Increased visceral fat
- Rising insulin resistance
- Changes in cholesterol
- Low-grade inflammation
These are not separate issues—they’re part of a metabolic shift that directly impacts blood pressure.
Hypertension is strongly linked with:
- Dyslipidemia
- Inflammation
- Endothelial dysfunction
- Weight gain
In other words:
Rising blood pressure is often an early marker of declining metabolic health.
Midlife often brings:
- Career pressure
- Aging parents
- Family demands with kids & teens
- Sleep disruption
Chronic stress → increased sympathetic (“fight or flight”) activity
→ higher heart rate and vascular tone
→ higher blood pressure
-
Sleep disruption (highly underrated)
Perimenopause is associated with:
- Night sweats
- Insomnia
- Fragmented sleep
Poor sleep is strongly linked to:
- Increased blood pressure
- Insulin resistance
- Weight gain
When should you start monitoring more closely?
Here’s the clinical reality:
- Hypertension is often completely silent
- Many women don’t know they have it until it’s advanced
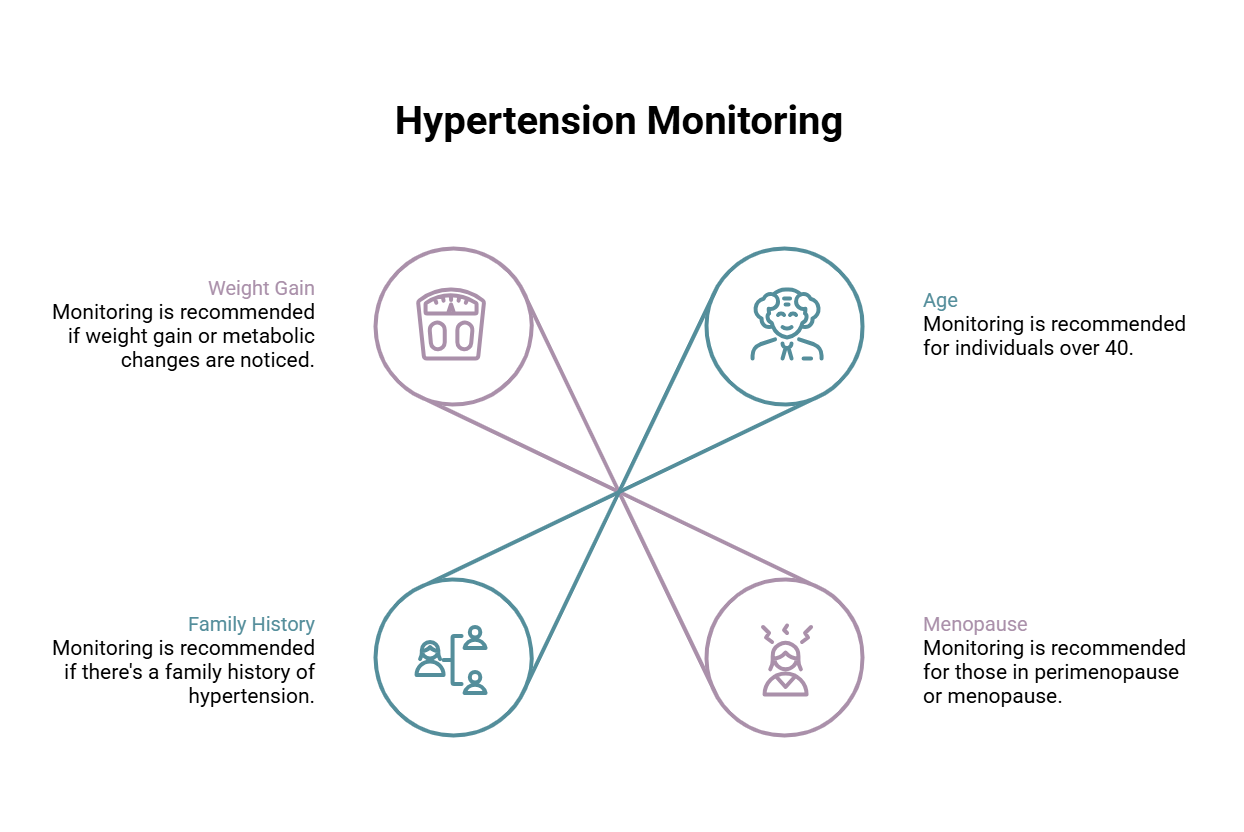
You should be actively monitoring if:
- You are 40+
- You are in perimenopause or menopause
- You have a family history of hypertension
- You’ve noticed weight gain or metabolic changes
Guidelines suggest:
- At least annual checks
- More frequent monitoring if readings are elevated
Why this matters: blood pressure and long-term health
This is not just about a number on a cuff.
High blood pressure is one of the strongest predictors of cardiovascular disease.
It contributes to:
- Heart attack
- Stroke
- Heart failure
- Kidney disease
After menopause:
- Cardiovascular risk rises significantly
- Blood pressure is a key driver of that risk
In fact:
- Postmenopausal women have a dramatically higher incidence of hypertension
- And a significantly increased risk of cardiovascular events
The deeper message: blood pressure is a signal
In your 20s and 30s, your body compensates.
In your 40s and 50s, it starts to reveal.
Blood pressure is not just a cardiovascular metric.
It is a window into your metabolic, hormonal, and nervous system health.
Simply Healthy, Simply Strong
If your blood pressure is rising in midlife, it’s not a failure.
It’s feedback.
A signal that:
- Your hormones are shifting
- Your metabolism is recalibrating
- Your cardiovascular system needs more attention
And the earlier you respond, the more preventable the long-term risks become. Book an appointment and we will work together to create a plan that is sustainable and will support your blood pressure and cardiovascular system.
References
- Li Z, Wang Y, Chen L. Perimenopausal syndrome and its association with hypertension. Front Cardiovasc Med. 2024;11:1298897.
- Lima R, Wofford M, Reckelhoff JF. Hypertension in postmenopausal women. Curr Hypertens Rep. 2012;14(3):254–260.
- American Heart Association. The connection between menopause and cardiovascular disease risk. Dallas (TX): American Heart Association; 2023.
- Mayo Clinic Staff. Menopause and high blood pressure: What’s the connection? Rochester (MN): Mayo Clinic; 2023.
- Johns Hopkins Medicine. Menopause and the cardiovascular system. Baltimore (MD): Johns Hopkins Medicine; 2022.
- Blood Pressure UK. Blood pressure, the menopause and HRT. London (UK): Blood Pressure UK; 2023.
- Office on Women’s Health. Menopause and heart health. Washington (DC): U.S. Department of Health & Human Services; 2025.