Midlife Sleep Disruption, Explained
If you’re waking between 2–4AM—wide awake, mind on, unable to fall back asleep—you are not alone.
This is one of the most common (and frustrating) experiences I hear from women in their 40s and early 50s.
And while it can feel random… it’s not. There are real physiological shifts happening beneath the surface.
Let’s walk through them—simply, clearly, and in a way that actually makes sense.
1. The Hormonal Shift You Can’t See (But Feel Everywhere)
Perimenopause is not a steady decline. It’s a time of fluctuation.
Two key hormones play a major role in sleep:
• Progesterone → calming, supports deep sleep
• Estrogen → influences serotonin, mood, and temperature regulation
As progesterone begins to decline, you lose one of your body’s natural calming supports at night.
The result:
- Lighter sleep
- More awakenings
- Less ability to stay asleep
At the same time, fluctuating estrogen can contribute to:
- Night sweats
- Temperature dysregulation
- Increased sensitivity to stress
Sleep disturbance is one of the most commonly reported symptoms during the menopausal transition, driven by both hormonal variability and changes in thermoregulation.
Bottom line: your brain is no longer being supported in the same way at night.
2. The 3AM Cortisol Shift
Your body runs on a rhythm.
In the early morning hours, cortisol naturally begins to rise to prepare you for waking. But in midlife, that rhythm can become less stable. Instead of a gradual rise, you may experience a more abrupt activation—enough to wake you.
This is often amplified by:
- Ongoing stress
- Poor recovery
- Overtraining
- Irregular sleep patterns
Disruption of the hypothalamic–pituitary–adrenal (HPA) axis has been shown to affect sleep quality and contribute to nocturnal awakenings.³
3. Blood Sugar Instability Overnight
This is one of the most overlooked drivers of 3AM waking. Your brain relies on a steady supply of glucose while you sleep.
When levels begin to drop—even subtly—the body responds by activating a stress response to maintain stability. This includes the release of hormones like cortisol and adrenaline. Those hormones are alerting by design. And in some cases, they are enough to wake you.
In midlife, this system becomes more sensitive.
Sleep disruption itself has been shown to worsen glucose regulation in women, particularly during the menopausal transition—creating a cycle that becomes increasingly difficult to break. The result? You fall asleep… But your body wakes you to stabilize itself.
[Need metabolic support? check out my blog on how to support midlife metabolic changes here ]
4. The “Tired But Wired” State
Many women in midlife are living in a constant, low-grade stress state.
Not always obvious.
Not always dramatic.
But persistent.
This leads to:
- A more reactive nervous system
- Difficulty entering deeper stages of sleep
- Early morning waking with a racing mind
You fall asleep… but your body doesn’t fully settle.
5. Alcohol: The Hidden Sleep Disruptor
A glass of wine may help you fall asleep faster. But it comes at a cost.
Alcohol:
- Fragments sleep
- Suppresses REM sleep
- Increases nighttime awakenings
Especially in the second half of the night—right around that 3AM window.
Even moderate alcohol intake has been shown to reduce overall sleep quality and increase awakenings.⁵
6. Histamine: The Underrated Piece
This is a more nuanced—but important—contributor.
Histamine is:
- A wakefulness-promoting neurotransmitter
- Also involved in immune responses
In some women, particularly during perimenopause:
- Histamine activity may increase
- Estrogen can influence histamine pathways
This can contribute to:
- Night waking
- A sense of alertness at odd hours
- Associated symptoms like headaches, flushing, or itching
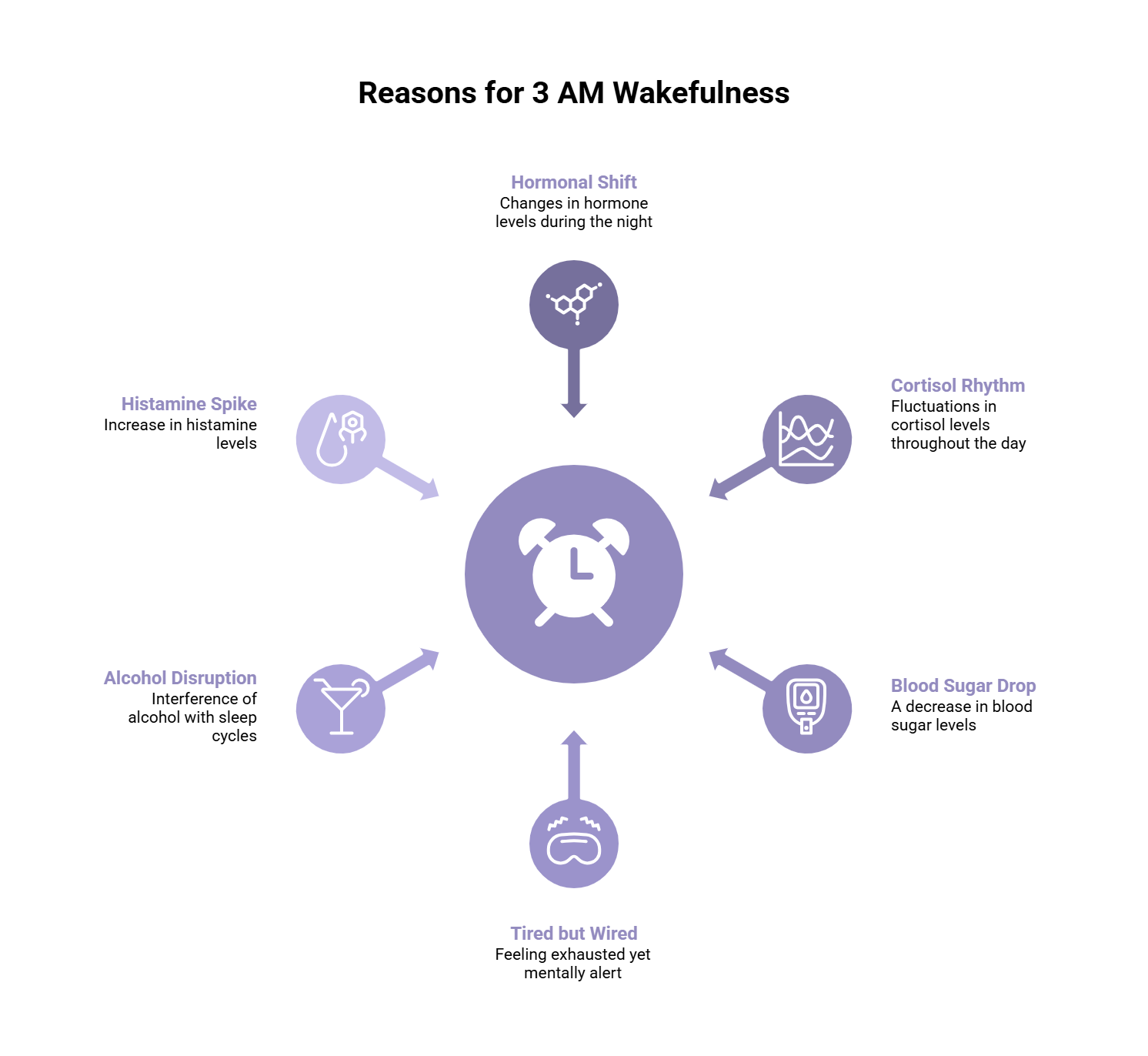
So What’s the Takeaway?
Waking at 3AM isn’t random.
It’s a signal.
A reflection of shifts in:
- Hormones
- Stress physiology
- Blood sugar regulation
- Nervous system balance
And most importantly… It’s something we can work with.
Not with a single supplement.
Not with a quick fix.
But with a targeted, physiology-informed approach.
Where to Start (Simply)
If you’re waking at 3AM, start here:
- Prioritize protein at dinner
- Reduce or remove evening alcohol
- Support a consistent sleep-wake rhythm
- Shift toward strength training over excessive cardio
- Build in intentional evening wind-down time
Small shifts.
Meaningful impact.
Final Thought
Midlife is not the beginning of decline. It’s a transition.
But your physiology is changing—and your strategy needs to change with it.
This isn’t about doing more. It’s about doing what works for your body now.
If you’re ready to go deeper, this is exactly the work I do.
If you’re looking for personalized support, you can also book an appointment and we’ll create a plan tailored specifically to you.
And if you’re interested in joining my upcoming perimenopause course, email me (lisatabrizi@gmail.com) and I’ll personally add you to the list.
Because the goal here isn’t just to get back to baseline.
It’s to feel clear, energized, and strong in this next phase.
Simply Healthy. Simply Strong.
References
- Baker FC, Lee KA. Menstrual cycle effects on sleep. Sleep Med Clin. 2018;13(3):283–294.
- Freedman RR. Menopause and sleep. Menopause. 2014;21(5):534–535.
- Buckley TM, Schatzberg AF. HPA axis and sleep interactions. J Clin Endocrinol Metab. 2005;90(5):3106–3114.
- St-Onge MP, et al. Sleep restriction and insulin resistance in women. Columbia University Irving Medical Center, 2023.
- He S, Hasler BP, Chakravorty S. Alcohol and sleep-related problems. Curr Opin Psychol. 2019;30:117–122.